Hematology
Hematology is a field that encompasses clinical and laboratory aspects of adult and pediatric diseases, both malignant and non-malignant. Common blood disorders include anemia, bleeding disorders such as hemophilia, blood clots and blood cancers such as leukemia, lymphoma and myeloma.
As reported by American Society of Hematology, whereas some blood disorders have benefited from progress in clinical research and development of new therapies, other areas have continuing challenges, such as disease heterogeneity and the complex combinations of genetic drivers that have evaded effective treatment to date. A wide variety of blood-related diseases – from malignancies such as lymphoma and leukemia to non-malignant diseases such as hemoglobinopathies, platelet and coagulation disorders, and orphan diseases of the hematopoietic system – continue to be associated with significant morbidity and mortality and demand attention to reduce their burden and improve quality of care worldwide.
In particular, the Lancet Haematology Journal in 2018 presented data from population-based cancer registries worldwide, with additional epidemiological analysis based on 54 countries with detailed records of age, sex, and subtype of leukaemia. The study highlights that haematological malignancies contribute substantially to disease burden in many countries. Leukaemia consistently appears in the top 30 list of total years lost of life due to illness for all socio-demographic index countries, except for the lowest index countries. Furthermore, when adding the contribution of other haematology-related diseases, such as haemoglobinopathies and haemolytic anaemias, maternal haemorrhage, and iron-deficiency anaemia, haematology-related diseases contribute substantially to global mortality and morbidity.
An important step forward for all haematology-related diseases is to develop early detection programmes tailored to local needs and resources, with prioritisation of allocation of resources. Taking into account the impact these diseases have in terms of economics can further help to make the case for political change and investment. With increasing urbanisation worldwide, focusing on improving the health of those who inhabit cities will help to reduce the burden from haematological diseases. Between now and 2025, the City Cancer Challenge will target over 200 cities to improve the health of at least 500 million people globally. Improving the access to health care and health systems in urban environments, will not only help people with haematological malignancies, but also go some way to addressing other haematological diseases. For example, the global burden of sickle-cell disease is set to rise as a consequence of improved survival in high-prevalence low-income and middle-income countries and in higher-income countries due to migration. Improving access to health systems and health services for these individuals will go a long way to decreasing morbidity and mortality from this disease.
Recent years have been key for the understanding of the fundamental biology of hematological diseases, in order to uncover genetic traits and possible risks factors underlying these sorts of conditions. These advancements have helped the rise of targeted and personalized treatments which are better tolerated by the patients in the long term.
The American Society of Hematology presents the efforts of the research community that is looking to emerging technologies and tools in the areas of precision medicine, epigenetics, gene therapies, immunotherapy, and regenerative medicine to identify areas that have strong potential to make a dramatic impact on patient care across a range of diseases.
Enhancing precision medicine efforts in hematology will require that sequencing technologies be adopted in drug discovery efforts, in the assessment of disease predisposition and response to therapy. Research on epigenetics, including its mechanisms and drivers, will elucidate highly valuable targets and lead to potentially transformative treatment regimens for hematologic disorders. New insights and technologies will optimize the use of stem cells and regenerative medicine, creating “designer” cells that will redefine approaches to the diagnosis and treatment of hematologic diseases.
Next-generation clinical studies will address important questions about emerging immunologic therapies but require an improved understanding of the basic biology of the immune system, including adaptive immunity, innate immunity, adjuvants, and tumor immune-surveillance.
In this scenario, a significant role has been played by chimeric antigen receptor (CAR)-T cell therapies for malignancies has already been approved for some types of lymphoma and leukemia, and clustered regularly interspace short palindromic repeats (CRISPR) gene therapy is now being studied in clinical trials for sickle cell and beta-thalassemia. The success of immunotherapy is due to a few advantages over classical treatments such as chemotherapy or radiation: it is focused on the immune system and often better targeted and it can lead to milder side effects than the classic treatments.
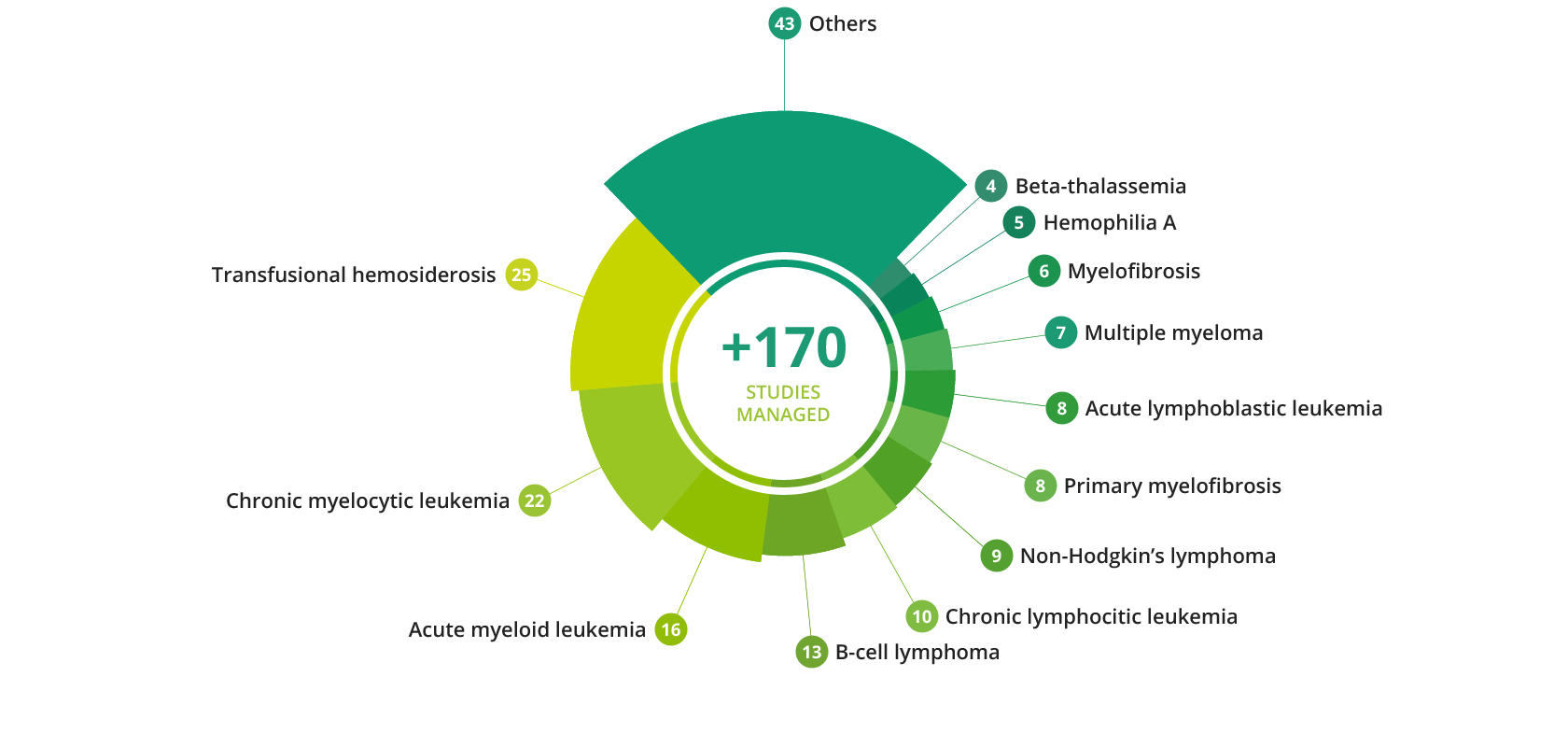
OPIS has managed over 170 studies in this therapeutic area and can therefore be considered a hematology-focused CRO, with the necessary expertise in novel molecularly targeted agents and know-how to provide and excellent service to the Sponsors that are tackling this ever-growing challenge in order to bring new therapies to the market.
Contact Us!
Whether you are Sponsor, a Clinical Research Professional or an Investigator contact us to learn more about how we can help.




